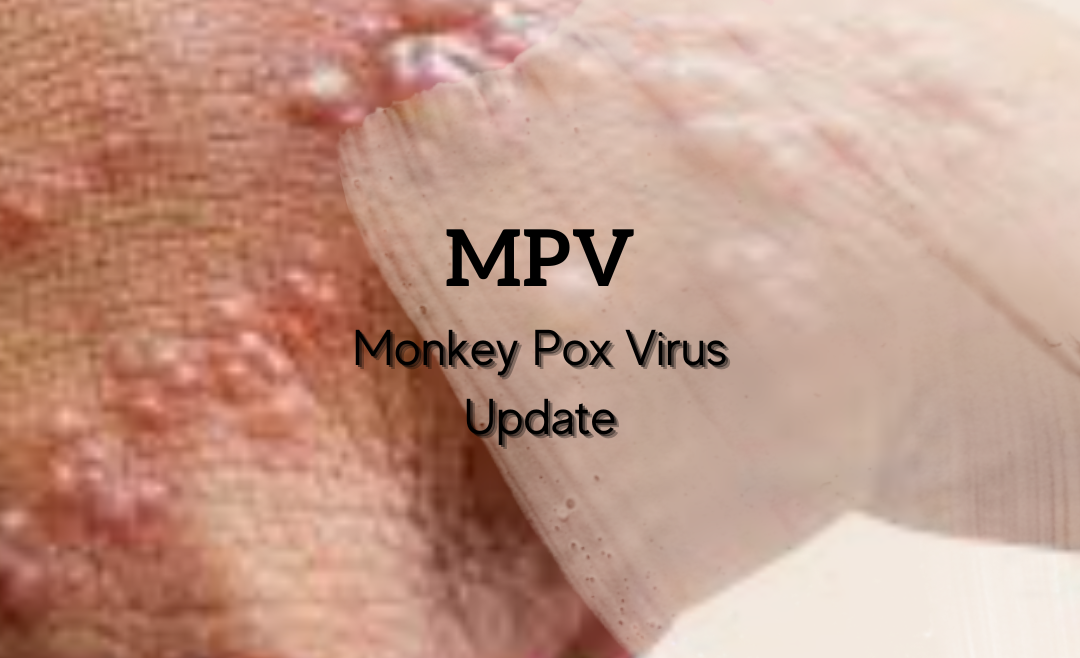
With the first confirmed case of Monkey Pox in the state of Florida being traced to Broward County, back in May, you would think more people would be talking about it locally.
The conversation IS robust; however, this seems to be limited to our local gay and bisexual community, particularly men who have sex with men. That is because one of the major modes of transmission is through skin to skin contact which is typical of sexual encounters; and immunocompromised adults are at a greater risk of increased severity of the virus.
Nonetheless, there are other modes of transmission that effect additional populations who are also at risk. It’s important to consider these additional risks when understanding the likelihood that you or a loved one may come into contact with the Monkey Pox Virus (MPV).
-
Prolonged Face to Face Contact
-
Direct Contact with Lesion Material (Scabs or Effected Skin with Rash)
-
Indirect Contact with Contaminated Material (Towels, Surfaces, Toys, Tables, Hand Rails, Fetish Props, Bedding, Clothing)
-
Mother to Fetus through Placenta
Compared to Covid-19, the mode of transmission seems to be much more direct; however, while there is no specific timeframe for how long MPV can live on surfaces, there has been a
CDC supported case of MPV surviving on surfaces in an unoccupied home for 15 days after the tenant left. A caveat to consider when disinfecting surfaces is that porous surfaces (think bedding and clothing, wood, the leather or fabric of a vehicle, or even certain types of stone countertops) can harbor viruses for longer than non-porous surfaces (think plastic, glass, or metal).
At this point in time, even as certain states declare a state of emergency due to Monkey Pox Virus, we do not need to be alarmed. However, with that being said, we need to stay vigilant, informed, connected, and prepared.
The problem with liminting the discussion to specific social communities is that other social populations may feel falsely reassured, wrongly associating the virus with a specific group of people, which can leave them blindsighted and create a weak link for potential superspreading that makes the situation more complicated to reel in.
Unfortunately, there is another subgroup of individuals who are also at increased risk for
severe outcomes which is not being talked about. That subgroup includes Children who are under 8 years of age, individuals who are pregnant or immunocompromised, and individuals with a history of atopic dermatitis or eczema due to decreased barrier protection.
If you do a google search, you will see frequent questions such as “What part of Florida has Monkey Pox?” or “Who in Florida has Monkey Pox?” The thought behind these questions is worrisome because it negates the fact that people travel and we are highly translocational beings even in light of the recent covid pandemic. The fact is that Monkey Pox is here. And we need to treat it as such.
Here’s What You Can Do:
- Make sure that you have a healthy dialogue with you sexual partner(s). If you are comfortable enough to have sex with them, you should feel comfortable enough to ask about any any recent illnesses, rashes, or sores on your partners body or your own body including the genitals and anal areas. You can never be too safe, so don’t be embarassed to look and see for yourself before taking someone’s word for it.
- If someone does have a rash or sores, avoid close contact which includes kissing, wrestling, hugging or sex. (If this pertains to a parent – child relationship, similar cautions are advised with a separate list of considerations.)
- Remember that animals can also be vectors of transmission, and avoid touching animals that reside with someone who has been recently ill, or presents with rashes and scabs.
- Avoid touching or sharing contaminated materials (bed linens, sex toys, towels, hair brushes, you name it.)
- Wash your hands consistently (We’ve been seeing alot of dishydrotic eczema so follow us on IG or FB for an upcoming video regarding some easy tips to avoid dry cracked hands in light of good hygiene practices.)
- If you are a parent or loved one who is caring for someone who has MPV, be sure to use Personal Protective Equipment (PPE) and contain and dispose of contaminated waste separately. Do your best to physically isolate the person while keeping them comfortable, in order to limit the amount of surfaces and objects that need to be disinfected.
If You Suspect you may have contracted the virus or you’re in a population that is particularly at risk
The first and most important step is to ISOLATE. Remember, this virus can take up to 2-4 weeks to run it’s course, so mentally and physically prepare yourself, and set up a support system with reduced and limited contact if necessary.
CONSIDER:
- Limit foods, spaces, and items shared with other household members.
- Do not allow anyone without an essential need to be in the home to visit.
- Use a separate bathroom from others who live in the same household.
- Ensure that eating utensils and soiled dishes are washed in the dishwasher or by hand with warm water and soap. Using a large container to do a bleach soak may help for individuals who do not own a dishwasher.
- Routinely clean and disinfect commonly touched surfaces and items. Do not forget counters, door knobs and light switches.
- Mask with a well fitting mask or N-95 when close contact with others at home is not avoidable.
- Avoid shaving over a rash to reduce spread of the virus to other unaffected areas of skin.
- Avoid contact lenses while on isolation to prevent potential infection of the eye.
For those at risk of a severe outcome from the virus
Follow
this link to find out where you can book an appointment for a vaccination. It’s better to get in line for a vaccination PRIOR to getting infected. With highest efficacy shortly after the second dose is administered within 4-8 weeks of beginning the series.
Remember, viruses do not exclude any population groups. We are all part of a community network and it’s our job to look out for our neighbors, friends, families and ourselves. We are all responsible for staying informed and connected.
If you found this article helpful, please share with someone who could benefit from this information. Let’s all do our part to keep the Pox in the Box!
Warm Regards,
Nicole Gentile, MMS, PA-C, CNT
Tags: atopic dermatitis, bisexual, broward county health, coronavirus, gay community, immunocompromised, infection, isolation, lgbtq, Monkeypox, monkeypox broward, monkeypox vaccine, orthopox virus, pediatric monkeypox, pregnant women, skin to skin, viral transmission, virus, what to do